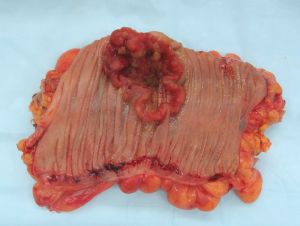
Colorectal cancer
Background
[[File:Pie chart of colorectal polyp etiologies.png|thumb|Epidemiology of colorectal polyps[1]40% - (2005). "Colorectal Cancer: Epidemiology, Risk Factors, and Health Services". Clinics in Colon and Rectal Surgery 18 (03): 133–140. DOI:10.1055/s-2005-916274. ISSN 1531-0043., CC0,</ref>
- Colorectal cancer is extremely common
Clinical Features
- Asymptomatic, frequently grow slowly for long period of time before symptomatic
- Lower GI bleeding (occult or visible BRBPR/hematochezia
- Fatigue, generalized weakness due to anemia
- Change in bowel habits, constipation, tenesmus in rectal cancer
- Obstruction if mass large enough (left colon > right)
- Abdominal pain
- Focal pain or Peritonitis if perforation
- Abdominal pain
- Signs/symptoms of metastatic disease (e.g. hepatomegaly, ascites, lymphadenopathy) may be initial presentation
Differential Diagnosis
Undifferentiated lower gastrointestinal bleeding
- Upper GI Bleeding
- Diverticular disease
- Vascular ectasia / angiodysplasia
- Inflammatory bowel disease
- Infectious colitis
- Mesenteric Ischemia / ischemic colitis
- Meckel's diverticulum
- Colorectal cancer / polyps
- Hemorrhoids
- Aortoenteric fistula
- Nearly 100% mortality if untreated
- Consider in patients with gastrointestinal bleeding and known abdominal aortic aneurysms or aortic grafts
- Rectal foreign body
- Rectal ulcer (HIV, Syphilis, STI)
- Anal fissure
LLQ Pain
- Diverticulitis
- Kidney stone
- UTI
- Pyelonephritis
- Ectopic pregnancy
- Infectious colitis
- Inflammatory bowel disease (Crohn's Disease, Ulcerative Colitis)
- Inguinal hernia
- Mesenteric ischemia
- Epiploic appendagitis
- Mittelschmerz
- Ovarian cyst
- Ovarian torsion
- PID
- Psoas abscess
- Testicular torsion
- Appendicitis
- Abdominal aortic aneurysm
- Herpes zoster
- Endometriosis
- Colon cancer
- Irritable bowel syndrome
- Small bowel obstruction
Anorectal Disorders
- Anal fissure
- Anal fistula
- Anal malignancy
- Anal tags
- Anorectal abscess
- Coccydynia
- Colorectal malignancy
- Condyloma acuminata
- Constipation
- Crohn's disease
- Cryptitis
- GC/Chlamydia
- Fecal impaction
- Hemorrhoids
- Levator ani syndrome
- Pedunculated polyp
- Pilonidal cyst
- Proctalgia fugax
- Proctitis
- Pruritus ani
- Enterobius (pinworms)
- Rectal foreign body
- Rectal prolapse
- Syphilitic fissure
Non-GI Look-a-Likes
Evaluation
- CBC, LFTs, coags if bleeding or signs of hepatic involvement
- CT abdomen- not definitive but may catch large mass or other alternative diagnoses
- Definitive diagnosis not likely to be made in ED, but suggestion of malignancy may be made on imaging if large mass seen
- Colonoscopy with biopsy
- Serum CEA
- Surgical pathology
Management
- Transfuse pRBCs prn for anemia
- Consult surgery for obstruction or perforation
- May also help coordinate outpatient diagnostic workup
Disposition
- Discharge if clinically stable
See Also
External Links
References
- ↑ Relative incidences:(2017). "Epidemiological aspects of endoscopic resections of colorectal polyps in patients at an endoscopy training center in the Santos region, Brasil". Rev Gastroenterol Peru 37 (1): 47–52. PMID 28489836.Malignancy risks:Tubular adenoma: 2% at 1.5cm - Minhhuyen Nguyen. Polyps of the Colon and Rectum. MSD Manual. Last full review/revision June 2019Tubulovillous adenoma: 20% to 25% - (2005). "Colorectal Cancer: Epidemiology, Risk Factors, and Health Services". Clinics in Colon and Rectal Surgery 18 (03): 133–140. DOI:10.1055/s-2005-916274. ISSN 1531-0043.Villous adenoma:15% - Alnoor Ramji. Villous Adenoma Follow-up. Medscape. Updated: Oct 24, 2016