Diferencia entre revisiones de «Harbor:ECMO CPR (ECPR)»
Sin resumen de edición |
Sin resumen de edición |
||
| Línea 85: | Línea 85: | ||
*[[File:Harbor UCLA ECPR RN Documentation and QI Form.pdf|thumb|Harbor UCLA ECPR RN Documentation and QI Form]] | *[[File:Harbor UCLA ECPR RN Documentation and QI Form.pdf|thumb|Harbor UCLA ECPR RN Documentation and QI Form]] | ||
*[[File:ED Attending ECPR Cannulation Check List.pdf|thumb|ED Attending ECPR Cannulation Check List]] | *[[File:ED Attending ECPR Cannulation Check List.pdf|thumb|ED Attending ECPR Cannulation Check List]] | ||
Live 8-25-2025; updated 4/2026 | |||
Revisión actual - 21:34 12 abr 2026
ECMO CPR (ECPR)
- ECPR involves Veno-Arterial ECMO cannulation of a patient during CPR for mechanical circulatory support as a bridge to cardiac catheterization or other definitive care for patients in refractory VFib/VTach.
- There are currently two EMS Agency-designated eCPR sites in the South Bay (Torrance Memorial and Long Beach Memorial Medical Centers).
Harbor UCLA ECMO-CPR First Phase Program
- This program is only for patients that are already in our ED and does not apply to the prehospial setting.
- Any EMS Radio calls about ECPR should be directed to designated EMS ECPR Receiving centers (Torrance Memorial or Long Beach Memorial Medical Centers) as part of standard radioroom procedures.
- Harbor-UCLA is in the process of becoming a to be a designated ECPR Receiving Center and anticipate we will become a designated center in 2026. While we are building our ECMO-CPR Program and moving towards ECMO CPR Receiving Center Designation we are currently offering this service during daytime hours Monday-Friday for in-house patients as a first phase program.
- This limited hour, first phase launch of ECMO CPR capabilities is only for patients already under the care of our ED with the goal of increasing our familiarity with ECMO care throughout the hospital and help us familiarize practice patterns.
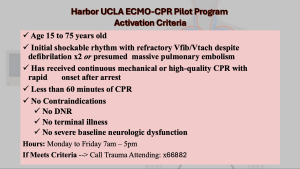
Harbor UCLA ECMO-CPR First Phase Hours of availability:
- Monday–Friday from 7 am to 5 pm
- If you feel patient should still be considered for ECPR outside of these hours please discuss case with the Trauma Surgery Attending (x66882)
ECPR Activation – Inclusion Criteria (all must be met):
- Age 15–75 years
- < 60 minutes since arrest
- Refractory/recurrent VF/VT (≥2 shocks) or presumed massive PE
- Continuous high-quality CPR
- No DNR
- No terminal illness
- No severe baseline neurologic dysfunction
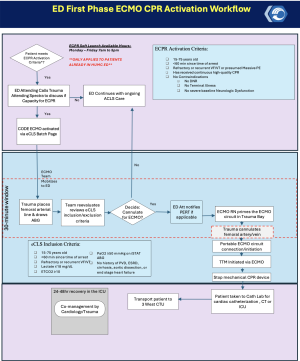
ECPR Activation process:
- If you have a patient who meets ECPR Activation Criteria, the ED Attending calls the Trauma Attending directly via spectra phone (x66882) immediately to determine if Harbor has capacity to care for an ECPR patient.
- As timing is important and avoiding delays to cannulation is critical, a simple “Hi Dr. ***, I have a patient who meets ECPR activation inclusion criteria and want to determine capacity to mobilize the ECMO Team.”
- It is very important that a prolonged conversation about the patient during this initial phone call does NOT take place. The only purpose of the phone call is to determine if we have hospital capacity and if so to activate the ECMO Team. Further discussion happens if ECMO team is mobilized and at the bedside.
- The Attending Trauma Surgeon will determine if there is hospital capacity to care for an ECPR patient.
- If they determine that there is capacity, they will ask you to have the clerk batch page the CODE ECMO pager.
- If they determine that there isn’t current capacity for ECPR, the ED team continues standard ALS efforts
- A Code ECMO batch page mobilizes the ECMO cannulation team (Trauma surgery, perfusionist, STEMI Team, ICU nursing and pharmacy) to the patient’s bedside.
- They will bring with them the ECMO circuit and cannulation supplies. Pharmacy will help provide required Heparin.
- If capacity is determined to be available, during ongoing ACLS, the ECMO team will place a femoral arterial line and obtain arterial blood gas for iSTAT Blood gas testing.
- The ECMO cannulation team and the ED attending will then review ECMO Life Support Inclusion Criteria Check List. The check list can be found at the trauma clerk desk and in trauma bays 1-5. Note these criteria includes additional factors beyond those used for initial activation File:ED Attending ECPR Cannulation Check List.pdf
- ECMO Life Support Cannulation Inclusion Criteria:
- Age 15-75 years old
- <60 min since time of arrest
- Refractory or recurrent VF/VT (persists despite defibrillation x2) or presumed Massive PE
- Lactate ≤18 mg/dL on iStat ABG
- ETCO2 ≥10
- PaO2 ≥ 50 mmHg on iSTAT ABG
- No history of PVD, ESRD, Cirrhosis, Aortic Dissection or end stage heart failure
- If the patient meets all the inclusion criteria and everyone agrees that the patient should receive ECPR-->
- The ECMO cannulation team will place the patient onto VA ECMO via bilateral femoral cannulas.
- Note: once the decision is made to cannulate the patient further further defibrillation is discontinued but other ACLS medications may be continued as well as ongoing CPR.
- Once the patient is successfully cannulated onto the ECMO circuit and flow on the circuit is started, CPR is stopped and the Autopulse/Lucas device is disconnected from the patient.
- Targeted Temperature Management is set via the ECMO circuit and time of TTM initiation is time of ECMO circuit start
- Once cannulated, the SICU / ECMO team assumes care of the patient, the patient is immediately admitted in PowerChart to the SICU and the patient is taken by interventional cardiology to the Cath-lab or directly to the SICU depending on clinical situation
- The ECMO cannulation team will place the patient onto VA ECMO via bilateral femoral cannulas.
- If the patient is determined to NOT be an ECLS candidate, ongoing ALS care is continued by the ED Team and the ECMO team will leave.
- For all ECPR Activations regardless if the patient undergoes cannulation an eCPR QI/QA document (AKA Nursing ECPR Documentation form) and ED ECPR Physician Powerform needs to be filled out File:Harbor UCLA ECPR RN Documentation and QI Form.pdf
- The Nursing ECPR documentation form is found at the Trauma Clerk Desk in the ECMO folders
- Completed ECPR QI/QA forms should be returned to the ECMO folder at the trauma clerk desk.
- The ED ECPR/ECMO PowerForm (PowerForms → ED Procedures → ECPR) is filled out by the ED physcian team leader for all activations, even if the patient is not cannulated.
What's My Role During an ECPR Activation?
- ED Physician Team:
- Identification of possible ECPR candidate
- Ensure high quality ACLS resuscitation and Lucas or AutoPulse Mechanical CPR device is utilized
- Once the decision is made to cannulate the patient, no further ALS medications, defibrillations are administered.
- Once patient is cannulated onto ECMO, CPR is stopped.
- Airway Management
- TEE (optional), if credentialed to assist with visualizing correct placement of the venous drainage catheter within the IVC/RA junction.
- Ordering Heparin 5000U IVP bolus, and Heparin 5000U/500cc NS to be brought to bedside (order set is being built currently)
- ED Attending:
- Discussion of ECPR capacity with Trauma Attending
- Review ECLS inclusion checklist with ECMO Team at Bedside
- Ensures the ED ECMO Powerform in powerchart about decision making to or not to cannulate is filled out. (This is done similar to logging procedures, ultrasounds)
- ECMO Team:
- Femoral arterial line placement and ABG acquisition
- VA Cannulation
- Autopulse ECMO circuit management
- SICU Attending Assumes immediate care of patient once ECMO cannulas are placed.
- Cardiology:
- Assist with mobilizing cath lab, reviewing ECLS inclusion criteria check list if present at bedside. Takes patient directly to Cath lab in most situations
- ED Nursing:
- Standard nursing care similar to any other ED resuscitation.
- Running iSTAT ABG on femoral Arterial line Sample
- Nurse who is in the documentation role will need to fill out the ECMO Documentation Nursing Form along side standard code/resuscitation sheet. **The ECMO Documentation Nursing and QI form is submitted to Annie Shih or Alex Grohmann, MD by submitting it to the ECMO folder in the OCN office.
- If decision is made to cannulate a patient onto ECMO, administration of heparin bolus prior to cannulation.
- Pharmacy:
- Assisting with ALS medications
- Rapidly obtaining 5000U heparin IVP to be administered prior to cannulation and compounding a 500cc NS bag containing 5000U Heparin to be used by the ECMO team when connecting cannulas on to the ECMO circuit.
Harbor UCLA ECPR Forms and Documents:
- File:Harbor UCLA ECPR RN Documentation and QI Form.pdf
- File:ED Attending ECPR Cannulation Check List.pdf
Live 8-25-2025; updated 4/2026