Diferencia entre revisiones de «Bacterial conjunctivitis»
Sin resumen de edición |
Sin resumen de edición |
||
| (No se muestran 10 ediciones intermedias de 6 usuarios) | |||
| Línea 1: | Línea 1: | ||
==Background== | ==Background== | ||
*Often due to staphylococcus or streptococcus | *Often due to [[staphylococcus]] or [[streptococcus]] | ||
{{Conjunctivitis DDX}} | |||
==Clinical Features== | ==Clinical Features== | ||
[[File:Bacterial conjunctivitis.jpg|thumb|]] | |||
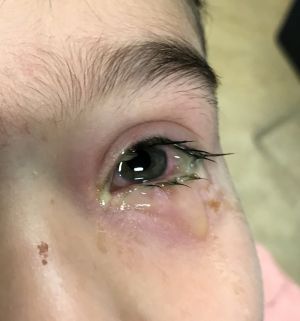
[[File:Bacterial conjunctivitis 2.jpg|thumb|An example of bacterial conjunctivitis with copious mucopurulent discharge.]] | |||
*Painless, unilateral or bilateral mucopurulent discharge | *Painless, unilateral or bilateral mucopurulent discharge | ||
**Often causes adherence of the eyelids on awakening | **Often causes adherence of the eyelids on awakening | ||
| Línea 8: | Línea 12: | ||
==Differential Diagnosis== | ==Differential Diagnosis== | ||
{{ | {{Unilateral red eye DDX}} | ||
{{Bilateral Red Eyes}} | |||
{{ | |||
==Evaluation== | |||
===Workup=== | ===Workup=== | ||
*Eye exam | *Eye exam | ||
*Fluorescein stain of cornea (especially in infants) to assess for corneal lesion | |||
*Culture: if severe | *Culture: if severe | ||
===Evaluation=== | |||
{{Clinical diagnosis of conjunctivitis}} | |||
==Management== | ==Management== | ||
| Línea 23: | Línea 29: | ||
==Disposition== | ==Disposition== | ||
*Discharge with ophtho follow-up (if no improvement) in 3 - 4 days | *Discharge with ophtho follow-up (if no improvement) in 3 - 4 days | ||
*Bacterial conjunctivitis is highly contagious. Patients may return to work or school after 24 hours of topical therapy and a reduction in discharge from eye(s). Advise good hygiene practices. | |||
==See Also== | ==See Also== | ||
| Línea 31: | Línea 38: | ||
<References/> | <References/> | ||
[[Category: | [[Category:Ophthalmology]] | ||
[[Category:ID]] | [[Category:ID]] | ||
Revisión actual - 17:13 4 feb 2026
Background
- Often due to staphylococcus or streptococcus
Conjunctivitis Types
Clinical Features
- Painless, unilateral or bilateral mucopurulent discharge
- Often causes adherence of the eyelids on awakening
- Chemosis is common
Differential Diagnosis
Unilateral red eye
- Nontraumatic
- Acute angle-closure glaucoma^
- Anterior uveitis
- Conjunctivitis
- Corneal erosion
- Corneal ulcer^
- Endophthalmitis^
- Episcleritis
- Herpes zoster ophthalmicus
- Inflamed pinguecula
- Inflamed pterygium
- Keratoconjunctivitis
- Keratoconus
- Nontraumatic iritis
- Scleritis^
- Subconjunctival hemorrhage
- Orbital trauma
- Caustic keratoconjunctivitis^^
- Corneal abrasion, Corneal laceration
- Conjunctival hemorrhage
- Conjunctival laceration
- Globe rupture^
- Hemorrhagic chemosis
- Lens dislocation
- Ocular foreign body
- Posterior vitreous detachment
- Retinal detachment
- Retrobulbar hemorrhage
- Traumatic hyphema
- Traumatic iritis
- Traumatic mydriasis
- Traumatic optic neuropathy
- Vitreous detachment
- Vitreous hemorrhage
- Ultraviolet keratitis
^Emergent diagnoses
^^Critical diagnoses
Bilateral red eyes
- Painful
- Painless
Evaluation
Workup
- Eye exam
- Fluorescein stain of cornea (especially in infants) to assess for corneal lesion
- Culture: if severe
Evaluation
Clinical diagnosis of conjunctivitis^
| Bacterial | Viral | Allergic | |
|---|---|---|---|
| Bilateral | 50% | 25% | Mostly |
| Discharge | Mucopurulent | Clear, Watery | Cobblestoning, none |
| Redness | Yes | Yes | Yes |
| Pruritis | Rarely | Rarely | Yes |
| Increased Likelihood | Presence of mucopurulent discharge; otitis media | Concomitant pharyngitis; an enlarged preauricular node; contact with another person with red eye | NA |
| Additional | Treatment: Antibiotics | Treatment: Hygiene | Seasonal |
Management
- Treatment for bacterial organisms is targeted toward S. aureus, S. pneumoniae, H. influenzae, Pseudomonas, N. gonorrhea, C. trachomatis
- Contact lens wearers should be given coverage for pseudomonas with one of the fluoroquinolone drops
Bacterial Conjunctivitis
- Counsel patient/family on importance of hand hygiene/avoiding touching face to prevent spread!
- Apply warm or cool compresses (for comfort and cleansing) every 4 hours, followed by instillation of ophthalmic antibiotic solutions
These options do not cover gonococcal or chlamydial infections
- Polymyxin B/Trimethoprim (Polytrim) 2 drops every 6 hours for 7 days OR
- Erythromycin applied to the conjunctiva q6hrs for 7 days OR
- Levofloxacin 0.5% ophthalmic solution 1-2 drops every 2 hours for 2 days THEN every 6 hours for 5 days OR
- Moxifloxacin 0.5% ophthalmic 1-2 drops every 2 hours for 2 days THEN every 6 hours for 5 days OR
- Gatifloxacin 0.5% ophthalmic solution 1-2 drops every 2 hours for 2 days THEN 1 drop every 6 hours for 5 days OR
- Azithromycin 1% ophthalmic solution 1 drop BID for 2 days THEN 1 drop daily for 5 days
- Chloramphenicol 0.5% ophthalmic solution 1 drop QID for 7 days
NB: levofloxacin is preferred for contact lens wearers for coverage of pseudomonas. Advise not to wear contacts for duration of treatment
Pediatric
Same topical regimens as adults; erythromycin ointment preferred in neonates and young infants
- Erythromycin 0.5% ophthalmic ointment applied q6hrs x 7 days (preferred in neonates/infants) OR
- Moxifloxacin 0.5% ophthalmic 1 drop TID x 7 days OR
- Azithromycin 1% ophthalmic solution 1 drop BID x 2 days then daily x 5 days
Chlamydial
- Doxycycline 100mg PO BID for 7 days OR
- Azithromycin 1g (20mg/kg) PO one time dose
- Newborn Treatment: Azithromycin 20mg/kg PO once daily x 3 days or erythromycin PO 50 mg/kg/day in 4 divided doses for 14 days [1]
- Disease manifests 5 days post-birth to 2 weeks (late onset)
Gonococcal
- Due to increasing resistance, CDC recommends dual therapy with Ceftriaxone and Azithromycin (even if patient is negative for Chlamydia).
- Ceftriaxone 1g IM single dose PLUS
- Azithromycin 1g PO one dose
- Newborn Treatment:
- Prophylaxis: Erythromycin ophthalmic 0.5% x1
- Disease manifests 1st 5 days post delivery (early onset)
- Treatment Ceftriaxone 25-50mg IV or IM, max 125mg or cefotaxime single dose of 100 mg/kg (preferred if the patient has hyperbilirubinemia)
- Also requires evaluation for disseminated disease (meningitis, arthritis, etc.)
Disposition
- Discharge with ophtho follow-up (if no improvement) in 3 - 4 days
- Bacterial conjunctivitis is highly contagious. Patients may return to work or school after 24 hours of topical therapy and a reduction in discharge from eye(s). Advise good hygiene practices.
See Also
References
- ↑ Zikic A, Schünemann H, Wi T, Lincetto O, Broutet N, Santesso N. Treatment of Neonatal Chlamydial Conjunctivitis: A Systematic Review and Meta-analysis. J Pediatric Infect Dis Soc. 2018 Aug 17;7(3):e107-e115. doi: 10.1093/jpids/piy060. PMID: 30007329; PMCID: PMC6097578.